Life & Art
Up close and personal with Covid-19
A foreign resident's first-hand perspectives on Taiwan's coronavirus pandemic response and healthcare system
By Douglas Habecker

For many years, Taiwan’s healthcare system has earned praise and plaudits as being one of the world’s best. As recently as February, it took the No. 1 spot globally among 93 countries for the second year in a row in online database Numbeo’s Health Care Index by Country 2020 survey. Other similar affirmation came with a No. 1 ranking out of 89 countries in CEOWORLD Magazine’s health care index survey, released in August 2019.
Good local healthcare has also been a factor in helping to propel Taiwan to the top as the world’s best place to live in both the 2016 and 2019 InterNations’ Expat Insider global surveys. Undoubtedly, it has also helped Taiwan attract a record-high number of over 414,000 medical visits by foreigners seeking treatment in 2019.
Despite these impressive statistics, however, the true basis for judging such a system is the experience it offers any individual who walks into a hospital or clinic seeking care. Add to this the extreme stress test of a global pandemic and you should end up with an accurate, tried-by-fire assessment with how Taiwan’s healthcare system really is and how it compares to systems in other nations.
I unexpectedly had such a personal opportunity—albeit an unexpected and unsought-after one—to get very up-close and personal with Taiwan’s medical system in March as Taiwan’s 50th official Covid-19 victim. In the weeks preceding this, I had keenly followed the daily local and global reports on the spread and impact of “Wuhan pneumonia”. Nevertheless, given Taiwan’s low number of cases and emerging success at containing the virus spread, I never imagined that I would have the dubious honour of becoming a topic for Minister of Health and Welfare Chen Shih-chung’s popular daily virus briefings.
The journey to that moment started on the eve of the 228 four-day holiday weekend when I was suddenly hit with chills, extreme fatigue and a slight headache behind my eyeballs while sitting in my office. Although a couple days of rest momentarily seemed to alleviate these symptoms, they came back and continued in the week ahead, joined a few days later by a sporadic dry cough, some nighttime fevers, and a strange altered sense of taste that left almost everything tasting unappetizing, to the point where it was a burden to eat even two meals per day. When I noticed around midweek that I was also coughing up some blood, I reluctantly decided it was time to seek medical care.
On 7 March, I drove to a Taichung hospital, walked into the emergency room and asked if I could get tested for Covid-19. However, the standard procedure called first for a chest x-ray, blood tests, a nasal swab and battery of questions from a doctor about my recent whereabouts and, particularly, any overseas travel. When all this was done, I was informed that because I had spent the past two months in Taiwan and there was little/no known local community transmission of the coronavirus, I didn’t fit the profile for Covid-19.
However, my lung x-rays did show some “cloudiness” and my bloodwork was not normal, so the doctor requested that I spent 2-3 days in the hospital for observation and treatment, in a private room to prevent potential infection of others. I was informed that my spacious private room (including an extra bed, sofa, desk and closet space) would cost NT$4,200 per night, not paid by National Health Insurance (NHI), which only covers shared rooms. I also would need to request and pay for any hospital food during my stay, as it was not automatically provided. These simple, but healthy, box-lunch-style Taiwanese meals were only NT$200-300 per day and largely unvarying—“hsi-fan” rice porridge for breakfast, fish for lunch, and pork or chicken for dinner, together with rice, vegetables, mushrooms and tofu.
Besides food, I quickly realized that I needed to provide any significant amenities, as the room only came with toilet paper, a small bar of soap, disposable hand towel and toothbrush, and packets of toothpaste and shampoo. Over the course of my stay, I came to deeply appreciate the helpful generosity of a few friends who helped purchase and deliver everything from extra underwear and T-shirts to books, dishware, candy and fresh fruit.
Over the next several days, I was treated with anti-flu medicine, antibiotics and other medications delivered by nurses who also hooked me up to IVs, took regular temperature and blood-pressure readings, asked me about things like my daily bowel movements, and provided “ice pillows” when I was running a fever. The doctor assigned to my case also stopped by once a day with updates and questions. It was her continued questions that prompted me to think of a one-day Taichung visit by four American friends—in Taiwan for three days on a journey between Washington State and Thailand—only three days before I began feeling sick. We had spent the day touring Taichung in my car and I now recalled that one of my friends had commented that he had some chills and didn’t feel too well over dinner that night.
I sent my friend’s wife a brief LINE message, asking how they had been doing since leaving Taichung and her reply was a bit alarming. In the days that followed their Taichung visit, my friend indeed had gotten sick with symptoms similar to the ones I was experiencing. His wife had also fallen ill a few days later, followed by a third member of their party. However, she added that none of them were seriously sick and that her husband actually seemed to have recovered.
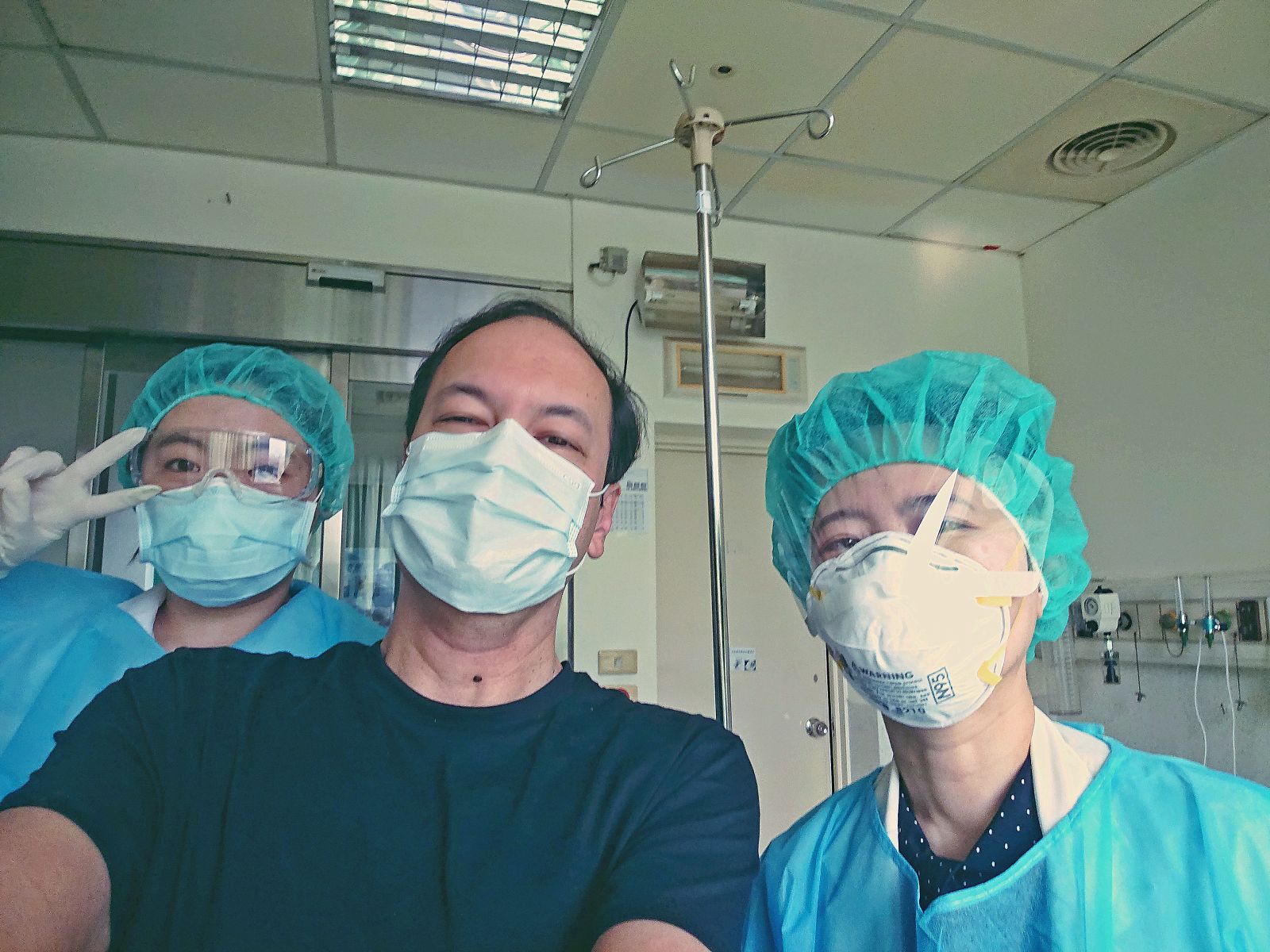
My mention of this news to my doctor immediately changed everything. A throat-swab Covid-19 test was ordered and my medical caretakers suddenly began entering my room in full personal protective equipment (PPE). Although the first test’s “weak positive” result wasn’t entirely conclusive, I received a call from Taichung City Government health officials, informing me that they had asked the hospital to immediately relocate me to a negative-pressure isolation room, which Taiwan’s government required all hospitals to install following the 2003 SARS outbreak.
At this point, another much-heralded and critical element in Taiwan’s Covid-19 success came into play—contact tracing. Via a series of phone calls, city health personnel began carefully reviewing my whereabouts and those I had any significant encounters with just before and after I began feeling ill. With my help, they also established a direct link to my four friends for further information regarding their time in Taipei, flights in/out of Taiwan and other details. What impressed me as much as their thoroughness was their calm courtesy, patience, understanding and discretion, which made the entire process much less stressful. They also reassured me that, outside of those individuals they would need to contact, my anonymity was being protected. Even the hospital I was staying at remained a well-guarded secret.
Also helping reduce my stress levels was the understanding, support and concern expressed by almost all of the above colleagues, friends and contacts that I informed at this point about my condition, despite the likelihood that some of them were now facing time in quarantine themselves. My entire office staff and some other individuals I’d spent significant time with were quarantined, with the remainder of my contacts asked to self-monitor their health and report any signs of Covid-19.
Two days after my initial test, a second test reconfirmed that I indeed had been infected with Covid-19, just after I received another message from Washington State informing me that my unwell American friend’s mother—who he spent a few hours with before flying to Taiwan—had just tested positive for the virus.
Meanwhile, much to the frustration of my four friends back in America, their hospital refused to test them because they didn’t meet the standard for symptoms (described literally as “being unable to complete a sentence without having to take a breath”). This was despite the fact that my friend’s wife by this time had a cough, tightness in her chest and fatigue and had lost her sense of taste and smell. In the end, they only managed to get tested through a personal connection to a doctor. They finally established that all four of them had been infected with Covid-19, although none were hospitalized nor experienced any serious complications.
This inability to conduct timely tests of possible coronavirus patients was a theme that would soon gain widespread media coverage across the US and contrasted the multiple Covid-19 tests I would receive during my Taiwan hospitalization. I was also surprised when the US hospital told my friend’s confirmed coronavirus-infected elderly mother to go home, self-isolate and only come back if her condition worsened, which it did a few days later when she had breathing problems that required further hospitalization.
By the standard of many other coronavirus sufferers, my own illness was relatively mild with most significant symptoms progressively disappearing during the first 10 days in the hospital, leaving only a very sporadic cough and the occasional feeling of mild pressure in my lungs. The most dramatic improvement was my taste buds’ sudden return to normality, accompanied by an almost insatiable appetite and deeper appreciation for almost everything edible.
Among the biggest challenges during my 19-day stay in the hospital were isolation and boredom. The much-smaller negative-pressure isolation room was protected from the outside world by a sliding glass door, small outer atrium that my healthcare providers would access through a heavy outer metal door. Although I fortunately did have my laptop computer and some books, repeated rotations between reading, online time, TV watching and staring out my large window did grow old after a while. Nevertheless, I also discovered the value of maintaining a daily routine that included some simple exercises. While I did maintain contact with a select group of relatives and friends, I intentionally chose to severely limit those I informed to avoid being bombarded with inquiries and messages that might stress and overwhelm me and interfere with rest and recuperation.
My daily contact with other human beings—always cloaked behind PPE—was limited to three daily visits by nurses to deliver meals, medication and fresh face masks and administer temperature and blood-pressure checks, plus a daily visit by my doctor. Given the well-publicized global PPE shortages, I was reminded of Taiwan’s abundance during every single visit, even when it was just a 20-second delivery of food and medicine. Once the glass doors had closed behind them, my caretakers would pause in the atrium to shed their body, head and foot PPE and throw it into a medical-waste garbage bin before departing.
Most of these brief encounters focused purely on medical needs, although as time went on, I appreciated efforts by my visitors to sometimes linger and engage me in lighter conversations. The nurses would also refill my drinking-water containers and deliver extra clothing, snacks, books and other requested items dropped off at the hospital by helpful friends. On one occasion, the nurses’ station surprised me by ordering and delivering the first coffee (a large Americano) I’d enjoyed in weeks.
Undoubtedly, my ability to speak Chinese made all my hospital interactions much easier although there were times when I struggled to ask and answer medical-related questions, which could be frustrating and, occasionally, worrying. It did leave me wondering how much different and more difficult the experience would be for a foreigner without such language skills. Not for the first time, I also sensed that local doctors are used to handing out diagnoses, treatments and medications without explanation, discussion or debate, unlike their western counterparts, more accustomed to patients who request detailed information, have often done their own research and may even want another opinion.
With the improvement of my condition, the second half of my stay saw more Covid-19 tests, as three consecutive negative results are required before one is declared coronavirus-free in Taiwan. After my first negative result, there was a bit of apprehension about getting a positive result, which would require the entire testing process to start over again. Fortunately that didn’t happen and my three negative results were followed by an evaluation of my case by local and central health authorities who cleared me to go home, although it took a further 2-3 days for the official discharge document to arrive at the hospital.
Nevertheless, I had no complaints, as Taiwan’s thorough process for giving Covid-19 patients a clean bill of health is proving to be superior to countries where patients are reportedly released untested when their symptoms improve or after a single negative test result (or, like the US, where some patients are not hospitalized at all). There is some conjecture that this may be a factor in a handful of reports regarding coronavirus “reinfections” or relapsed patients in other places.
The time of my discharge was uncertain, pending the arrival of the government’s release document. However, on the morning of 26 March, the room intercom crackled to life and the nurse informed me I could go home. This somewhat anticlimactic conclusion to my battle with Covid-19 saw me packing up and—for the first and only time—hitting the big red button that opened the glass sliding door and walking out the big metal door beyond that.
Before leaving, I had to go downstairs to the hospital cashier and pay for non-NHI expenses totaling over NT$30,000. Although Taiwan’s Central Epidemic Command Center covered my Covid-19 related costs (including the isolation room) once I tested positive, I had to cover the private room I stayed in prior to testing as well as food and a few other expenses. After paying my bills, it was just a few steps to the door and outside where I felt the sun and breathed fresh air for the first time in almost three weeks.
In the days and weeks since then, I’ve continued to practice social distancing and my own version of a half-quarantine—working more from home and going out at quieter hours—partly out of sensitivity to the possible fears of my office staff plus the neighbours who may have suspected that I was Covid-19 patient No. 50 despite my government-protected anonymity. Physically, I’ve felt about 90% normal and almost immediately resumed weekend bike trips into the countryside without much difficulty.
Today I appreciate almost everything, from food and time with friends to personal freedom and sunshine, a lot more than I used to. Most of all, though, I’m thankful to have been in Taiwan during this global and personal battle with Covid-19. This nation’s healthcare system isn’t perfect but recent and past experiences leave me fully affirming its No. 1 status.
Douglas Habecker is a writer, Compass Magazine co-publisher and current Taichung AmCham chairman